- Home
- Weddings
- Portraits
- Journal
- Contact
- Idle champions of the forgotten realms ahk script
- Fallen leaf campground reservations
- Download imovie for mac 10-7-5
- Time zones in australia
- Iphone won t send sms to android
- Itranslate pro apple watch change language
- Desktop pins
- Kid3 edit format tag
- Key by key steps to fix windows 7 bsod stop error code 0xed
- Target photo print
- Halloween costumes baby ninja turtles
- Spinal fluid
- Ertl jibber jabber doll
- Review and comparison stockmarketeye
- Icedrive plan
- Oxford advanced learners dictionary of current english

I might measure the pressure of the spinal fluid and collect several tubes for analysis. Then, I’ll remove the center of the needle, and spinal fluid will begin to flow. I’ll insert the needle, using my experience to ensure I find the precise location. We’ll continue our friendly conversation – How was your weekend? How are your grandkids? How’s this weather? Generally, it only goes halfway in, and you won’t feel a thing. You might be surprised by how long it looks, but don’t let that scare you. I’ll head back into that same area, this time using a spinal fluid needle. The nurse may also help you keep your knees up high. We’ll chat, and I’ll lay out the spinal fluid collection tubes on my sterile tray. I’ll wait a couple of minutes for the numbing medicine to kick in. But it really is no big deal because you’re already numbed. You’ll feel some pressure, and if there is any discomfort, I can take the needle out, get a little more lidocaine, numb some more, then continue the procedure.
SPINAL FLUID SKIN
From here, you won’t feel anything.Īfter the surface of the skin is numb, I’ll take a slightly bigger syringe and, with my hand on your back, I’ll gently inject the area where the spinal needle will go. In all honesty, this is the most painful part of the whole procedure, and it’s little more than a tickle. I’ll put on my sterile gloves and use 1% lidocaine and a very thin, 30-gauge needle to numb a small area of skin. You won’t be exposed during the procedure. I’ll surround the area with sterile drapes – essentially paper towels – by placing one on top of you and tucking one underneath you and into your pant waist. We can use an alcohol-based disinfectant. If you’re sensitive to iodine, that’s no worry. Then, I’ll use an iodine-based solution called Betadine® to scrub your skin and remove any surface bacteria. I like talking to my patients, and I want everyone to feel relaxed. I’ll put on some clean gloves, and we’ll start chatting. At this point, you can feel reassured knowing that, with a properly performed lumbar puncture, there is no risk of piercing the spinal cord. I’ll put my hand on the top of your hip bone (the iliac crest) and feel for what’s called the L4-L5 interspace. The nurse can help you get in position if needed. Instead, I ask you to lie on your side with your knees as close to your chest as possible. I don’t use fluoroscopy – a real-time X-ray guidance tool – to perform lumbar punctures, as I don’t find it necessary most of the time. Drink plenty of water beforehand, and I’ll have a much easier time drawing your spinal fluid. To make your spinal fluid examination as comfortable as possible, I recommend arriving at my clinic well-hydrated. The more you know, the less scary it seems, right? So, let’s unpack the procedure from start to finish. Demystifying the spinal examination procedure Just like a blood, you can perform many different tests on spinal fluid. Lumbar punctures measure distinct aspects of spinal fluid, such as the pressure it’s under, infections, and other biomarkers. It’s clear and could easily be mistaken for water.
Right now, you have about 100 to 150 ml of spinal fluid in your spinal and skull cavities.ĭespite what you might imagine, healthy spinal fluid isn’t pus-like or filled with blood. It also surrounds these parts of the central nervous system which seem to float in the fluid.

Once secreted by specialized tissue called choroid plexus, CSF passes through channels and aqueducts in the brain and brainstem.
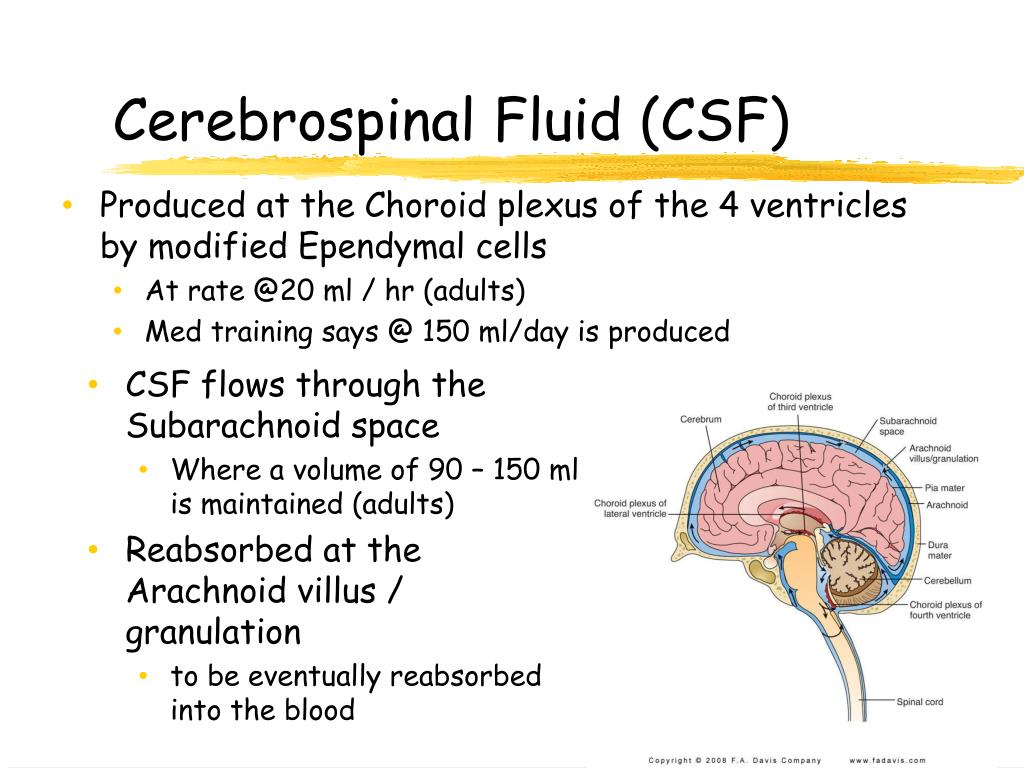
But first, what is spinal fluid, and why might a neurologist like me request a spinal fluid examination? What is spinal fluid?Ĭerebrospinal fluid (CSF) is a biologically active tissue, produced in the center of the brain. To ease your nerves, I’m going to walk you through exactly what to expect during this routine procedure. Spinal fluid examinations, or lumbar punctures, as I sometimes call them (I avoid the phrase ‘spinal tap,’ as it isn’t accurate and terrifies some folks), are only a little more involved than your standard blood test. I know the procedure sounds painful and high-risk, but trust me, it’s anything but. I’ve been practicing as a neurologist and medical doctor since the early 1990s, and I’ve done thousands of spinal fluid examinations.

